VNJ Articleschronicclinicalwound
23 August 2022
Approaches to wound management – Part 3 Treatment of a chronic, necrotic neck wound in a stray cat by Caroline Calder
ABSTRACT: This is the third in a series of articles that charts the progress of wound healing using advanced wound management. The patient presented as a stray, therefore raising the issue of costs of treatment. This case covers manual, medical and surgical techniques to achieve wound healing in the presence of chronic necrosis. The wound was extensive and in a difficult location and this affected the decisions made on how to manage it.
Pedro was an adult entire, male, DSH cat presented as a stray. A large necrotic neck wound was evident. The cause was unknown but, owing to the degree of necrosis, it was suspected that the wound may have been present at least one week.
This article charts the step-by-step process taken to debride the wound, and encourage healing; and then the surgical repair of the wound through to a successful rehoming after attempts to locate the owner were unsuccessful.
Case diary
Day 1
A large, chronic, necrotic wound was evident on the left lateral neck ventral to the ear. There was a strong odour. The wound measured 6.5cm long x 5cm wide. Loose, unviable, necrotic tissue was present (Figure 1).
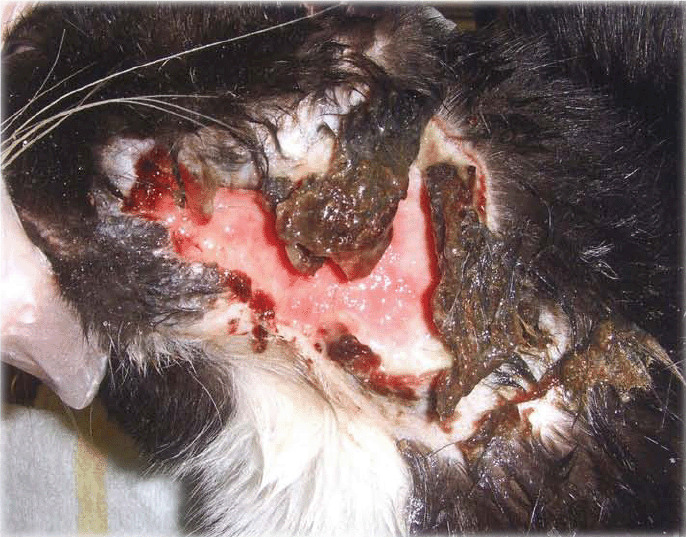
Figure 1: Initial presentation, loose necrotic tissue present
The wound was clipped, cleaned and flushed with saline and the loose necrotic tissue debrided manually with scissors (Table 1). The majority of the wound edges were necrotic (Figure 2).

Figure 2: Day 1. Post manual debridement of necrotic tissue As there was no owner involvement, it was decided to treat the wound conservatively in the initial stages. Manuka medical honey (Activon, Advancis Medical) was applied to the wound and it was left open. A long-acting injection of amoxicillin (Duphamox LA, Pfizer) was given.
As there was no owner involvement, it was decided to treat the wound conservatively in the initial stages. Manuka medical honey (Activon, Advancis Medical) was applied to the wound and it was left open. A long-acting injection of amoxicillin (Duphamox LA, Pfizer) was given.
Day 2
Although very nervous, the patient was doing well and had not interfered with the wound. It was decided to determine his FeLV/FIV status, owing to the high risk of contracting these diseases as an entire male stray. He was negative for both.
Had he been positive this would have affected the prognosis. It would have reduced his chances of being homed as he would have had to go to an indoor, single-cat household to prevent cross infection to other cats. Euthanasia might have had to be considered.
He was given a worm and flea prevention treatment – milbemycin (Milbemax, Novartis) and fipronil/(s)-methoprene (Frontline, Merial). The wound was cleaned and assessed (Table 1) and further necrotic tissue was debrided manually.
A honey-impregnated mesh dressing (Activon Tulle, Advancis Medical) was cut to size and applied over the wound. A secondary hydrophilic foam dressing (Advasorb Plus, Advancis Medical) was stapled in place over the honey dressing and a head bandage was used to secure everything (Figure 3).

Figure 3: Day 2:Head/neck dressing in place
Day 3
The patient was tolerating the dressing reasonably well, but had begun to scratch at it. A repeat injection of long-acting amoxycillin was given.
Day 4
The dressing had slipped, so it was removed. The honey tulle had successfully debrided the remaining necrotic tissue, leaving healthy granulation tissue (Figure 4). The wound was cleaned and assessed (Table 2) and redressed as Day 2.

Figure 4: Day 4: Necrotic edges fully debrided, healthy granulation tissue

Day 5
The patient had been interfering with the dressing and it had slipped again, so it was removed and redressed as before but using topically applied manuka honey rather than the tulle.
Day 6
The dressing had slipped again. The tolerance and suitability of long-term head dressings was now in question; and because the wound was so extensive, healing would take some time and dressings might have been required for several weeks. As this involved s
ignificant cost, and no owner had come forward, it was decided to repair the wound surgically – whilst the patient was being castrated under anaesthesia – which would decrease the healing time dramatically.
The wound was debrided and repaired using absorbable monofilament polydioxane (PDS, Ethicon) subcutaneously and a non-absorbable nylon (Supramid, SMI) in the skin. The wound was extensive and under some tension (Figure 5). There was a risk of wound breakdown postoperatively, so the patient was given further amoxycillin and an injection of the non-steroidal anti¬inflammatory (NSAID), meloxicam (Metacam, Boehringer).

Figure 5: Day 6: After surgical debridement and closure of the wound
Day 7
The patient had become a much happier cat (Figure 6)! Previously he had been destructive in his kennel when left overnight and was nervous and unhappy. He had now become very happy and affectionate, so he was taken to a ‘foster home’ to be cared for whilst his wound healed.

Figure 6: Day 7: Day after surgery, a much happier cat!
Day 8
An injection of the long-acting antibiotic, cefovecin, (Convenia, Pfizer) was given.
Day 10
The wound was healing well (Figure 7). The cranial end was oozing slightly, so the fosterer was advised to clean it with saline twice daily and to apply honey topically three times daily. The patient had settled well into his foster home and was very sociable with the fosterers and their other pets.

Figure 7: Day 10: Wound holding together well.
Day 12
The patient had been scratching at the wound and the cranial end had opened up slightly (Figure 8). The sutures, however, were holding in place.

Figure 8: Day 12: Minor breakdown on wound at cranial end
Day 17
The sutures were removed. The wound had healed very well with just some scabbed areas (Figure 9). The fosterer was advised to continue bathing the wound and to apply a hydrogel three times daily – Cutimed gel (BSN Medical) was used.

Figure 9: Day 17: Sutures were removed, wound healed well
Day 26
The patient was adopted by one of our clients and his vaccination course was started. The wound had fully healed and only scar tissue remained.
Day 43
Hair regrowth was present (Figure 10) and Pedro had settled into his new home.

Figure 10: Day 43: Fully healed!
Discussion
Because of the extenuating circumstances when dealing with a stray, this case was more than just a standard ’wound case’. The patient s homeless status affected how it was managed because it placed the practice in a difficult situation as far as costs of treatment were concerned and the difficulties of
rehoming cats meant that his future was uncertain. Fortunately, donations were made by some of our clients, which covered the costs of his care.
Long-term bandaging can incur high costs versus a one-off surgical repair, and this was taken into account when making decisions regarding managing the case. The location of the wound, and whether the patient would tolerate dressings in the long term, added to the practicalities under consideration.
Initial conservative management using the manuka honey was very successful at debriding the wound and encouraging healthy granulation tissue prior to surgery. However, the risk of breakdown postoperatively was still high and further surgery might have been necessary. Fortunately that was not the case as the surgery was successful and greatly reduced the healing time.
The benefits of adopting a moist wound management approach are easy to see. Results can be obtained very quickly when dealing with issues like the initial necrosis (Day 1), minor wound breakdown (Days 10 &12) and postoperative scabbed areas (Day 17).
Outcome
After Pedro had surgery he became a different cat. The open wound had obviously been affecting him far more than was realised. He became very affectionate and settled into his foster home immediately. He was an ideal candidate for rehoming, and one of our clients adopted him – a truly happy ending!
Author
Caroline Calder RVN MBVNA

Caroline qualified in 2001 after attending Myerscough College, whilst working in Carlisle. For the last six years she has worked at a small animal practice in Durham. Since attending a CPD course in 2010, she has developed a keen interest in wound management.
To cite this article use either
DOI: 10.1111/j.2045-0648.2012.00223.x or Veterinary Nursing Journal Vol 27 pp 366-369
Veterinary Nursing Journal • VOL 27 • October 2012 •